Thanks as always to Dr. Mike Silverman, Chair of the Department of Emergency medicine at Virginia Hospital Center, for these helpful updates!
Friday Night Update from the ER in Arlington, VA
I’m not on the patient side of healthcare very often, but I have been the last couple of days. My wife had outpatient surgery yesterday (she’s okay and recovering). She did not need to get a COVID test beforehand which was great. She did have to bring her vaccine card with her. All good. What I found weird was that the surgi-center did not allow family to wait in the waiting room. Instead, I dropped her off, came home, and waited for a phone call. There’s a lot of waiting before surgery and I’m sure she would have liked some company. I also would have liked to have spoken to the surgeon beforehand and immediately afterwards (he did call but it’s not the same as being there face to face). I’m a little surprised that 2 years into COVID and Omicron in the rear-view mirror, some places are still operating like 2020.
In the ER, we have a similar battle with certain psychiatric hospitals who have closed beds because of COVID, thus exacerbating a bed availability problem for a disease state that was already experiencing capacity issues prior to the pandemic. Again, just like everyone else has adapted to get back to business, my expectations for healthcare organizations are at least as high as school and businesses.
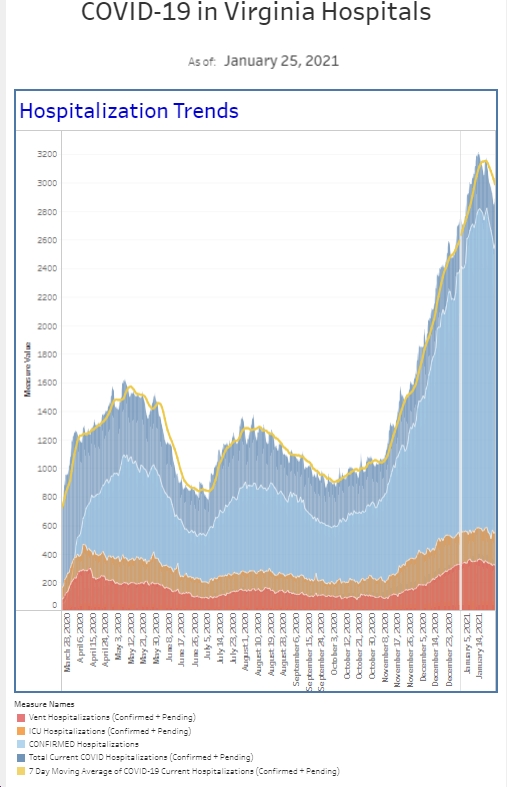
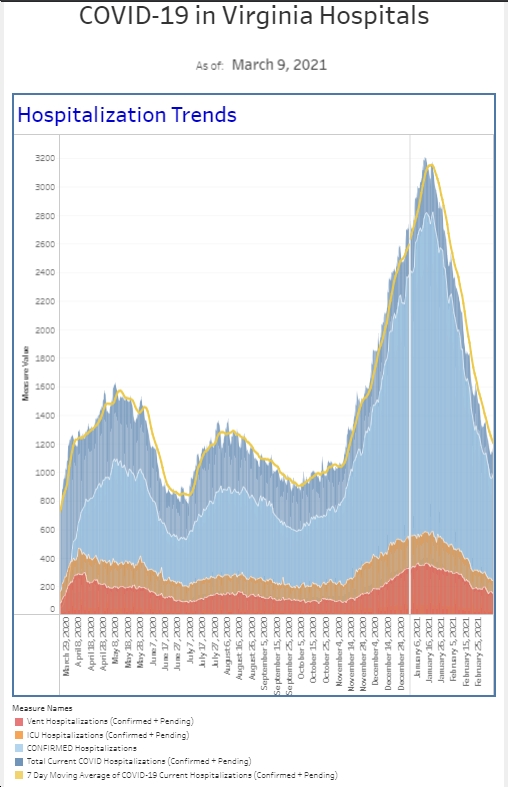
I had another week where I didn’t personally see any COVID patients in the ED. We’re still not back to our typical lull we see after surges end but each week, we’re a bit closer. The hospital numbers are down a touch compared to last week but holding steady. The number of cases we diagnose in the ER has dropped as well, particularly for the symptomatic patients we test. Our percent positive rate for symptomatic patients is down to 10% (which is the lowest it’s been since November) and it’s not uncommon to have a 24 hour period where we don’t diagnose anyone with symptomatic COVID. This is the 6th consecutive week with an improvement in this metric. Our asymptomatic screenings also had a slight decrease in percent positivity and drop in total cases. However, in terms of total cases we’re diagnosing in a week (separate from people who are positive and come in for worsening symptoms), we’re not back to the pre-Omicron lull yet. Our overall percent positivity rate is just under 7%.
There are some interesting articles that came out this week. First was a study out of Henry Ford Health System. Researchers looked at the number of admissions for alcoholic hepatitis between May-September 2020 and compared it to previous years. As has been previously reported, alcohol sales rose 54% in the first week of the pandemic alone and there is other data that suggested alcohol use increased in the early months of the pandemic. Alcoholic hepatitis is a type of liver disease caused by heavy drinking. Researchers found “in those five months of 2020, 93 patients were hospitalized with alcoholic hepatitis, an average of 18.6 a month. That was 50% more than the 12.2 average for the same months between 2016 and 2019.” More than 120,000 people a year are hospitalized for alcoholic hepatitis and the 28-day mortality rate is 26%. Although 20 patients a month may not sound like a lot across a hospital system, the 50% increase is substantial and concerning.
There’s a lot to be said about natural immunity and/or vaccination. As I look at the studies and try to learn more, it’s clear that it’s very complicated. It’s also clear to me that not getting vaccinated because you’d rather get COVID (and risk consequences) so you can have natural immunity is not a good game plan for society. Here’s what I can put together.
For patients who have had COVID (natural immunity), an Israeli study suggests that the quality of the antibody’s performance is better than those who have antibodies secondary to vaccine. This could explain why patients with natural immunity get reinfected less often compared to vaccinated patients who get infected a first time. One key caveat from the reinfection study is it didn’t include patients infected during the Delta or Omicron surges.
There were a couple of studies in the NEJM this week looking at natural immunity +/- vaccination. Natural immunity AND 1 dose of vaccination is better than natural immunity alone and provides longer protection than vaccination without natural immunity. However, for natural immunity, reinfection rates were much higher during the Omicron surge than previous variants and the reinfection rate is 4x higher for those with natural immunity who are unvaccinated.
In a new comprehensive review out of the UK that looked at data from 15 studies, vaccination also appears to reduce the risk of getting long COVID and improves long-COVID symptoms for those who were unvaccinated when infected.
What does all this mean to me? If you’re unvaccinated and get COVID, you’re more likely to require hospitalization or die from COVID than your vaccinated peers. The risk of myocarditis is higher from COVID than the vaccine. With that said, if you’ve had COVID and have natural immunity, you’re less like to get reinfected if you’ve had one dose of the vaccine. At this time, there does not appear to be benefit for further dosing, though we’re waiting on studies during Omicron as well as more time to go by to evaluate duration. Vaccination with natural immunity (in either order) is the most protected you can be at this point, but I certainly can’t and won’t recommend anyone who is vaccinated go out and try to get COVID. And I continue to recommend vaccination if you’re not currently vaccinated.
There are several expert opinions suggesting that perhaps 75% of Americans are immune to COVID at this point due to the vaccine/booster and/or natural immunity. Though one model (IMHE) estimates a range of 63-81%. This is much higher than we’ve had prior to other surges and hopefully paves the way for a return to normal and less disruption during the next variant surge (which seems inevitable). There are still 100,000 new cases a day and 2000 people/day dying so we’re not done with COVID, but we are potentially better equipped to move forward. The new oral medications could certainly be a game changer. This med was very hard to get when it first came out but I’m hearing there is some availability now. There’s still a lot to learn about vaccine duration and whether additional boosters will be necessary.
We also still need a vaccine for those <5 and we also need better mask guidance from the CDC. It’s not over but I am looking forward to spring.
The Coronavirus is not done with us yet.
Science matters. Get vaccinated (or your booster). Wear a mask.
Mike