Thanks as always to Dr. Mike Silverman, Chair of the Department of Emergency Medicine at the Virginia Hospital Center in Arlington, for these superb updates!
Friday Night Update from the ER in Arlington, VA
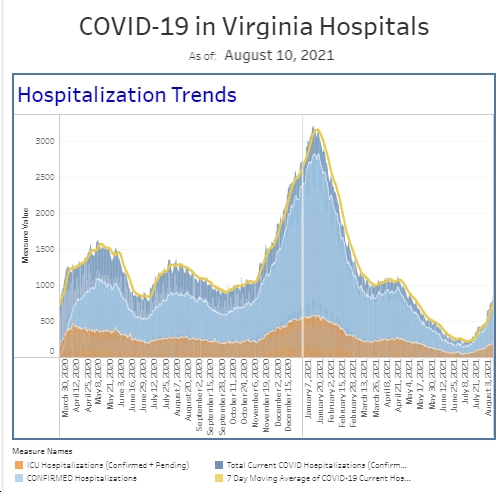
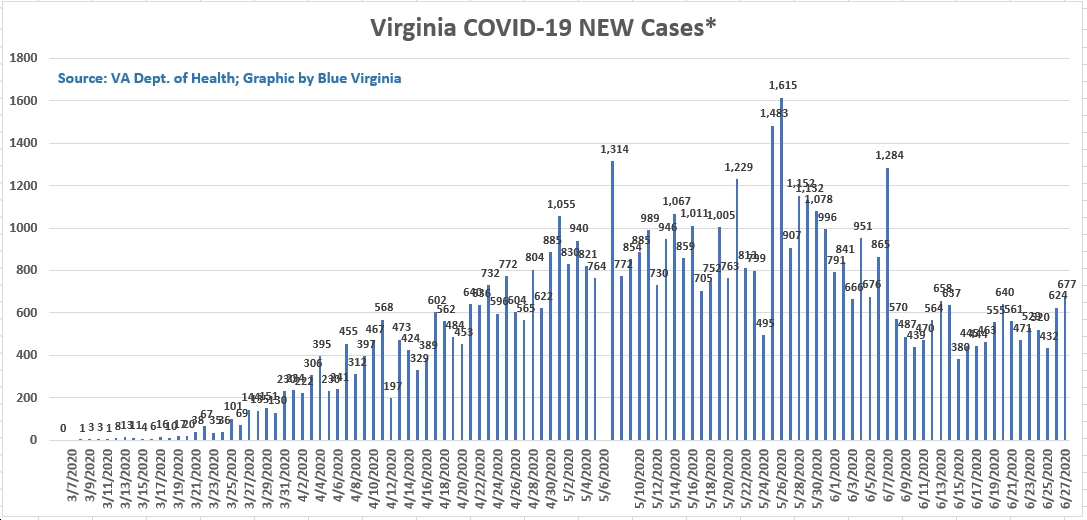
Since I’m hoping everyone is more focused on family and the holidays than reading this, let’s get right to it. ER volumes have been down a bit over the last week or so. Although I don’t have updated flu and RSV numbers from our lab, subjectively I can tell you we’re seeing less of these patients (though both are clearly still around). As an added benefit, the drop in RSV cases has made it a little easier to transfer critically ill pediatric patients to children’s hospitals. The CDC still classifies Virginia as having “very high” influenza like activity and COVID is up nationally, but our numbers in the ER look similar over the last couple of weeks—clearly higher than a month ago, but not the Omicron surge we had a year ago. Interestingly enough, I worked last evening on our main side (with the sicker patients) and a third of the patients I saw had COVID. That’s a bit of the problem of a small sample size (each doc working typically sees 8-12% of the day’s total patients). Although I saw a lot of COVID and some were pretty sick, the reality is that <10% of our patients have COVID. On the hospital side, I actually said “wow” this morning when I looked at the data. We currently have about twice as many hospitalized COVID patients as we’ve been running, including having several in the ICU. We’re not approaching our max numbers from earlier in the pandemic, but the numbers are consistent with what’s going on nationally—more people are requiring hospitalization.
If a dose of medicine is good, then more must be better? Steroids, specifically dexamethasone, turned out to be a game changer in the management of hypoxic, hospitalized COVID patients. But in a study published online this week, it turns out that “higher-dose corticosteroids increased the risk of death in patients with COVID-19 and hypoxia, compared with usual care that included low-dose corticosteroids.” The study looked at “over 1,200 patients, 18% of those randomly assigned to higher-dose dexamethasone died within 28 days compared with 12% of those assigned to usual care,” and “more patients in the higher-dose group required invasive mechanical ventilation.”
Studies show that there are clear benefits to getting your bivalent (updated) booster shot. Published by the CDC about a week ago, boosters are “reducing the risk of hospitalization by roughly 50 percent compared with certain groups inoculated with the original vaccines.” This increased to 73% for those over 65 years old. Another study “which included data on 93,830 adults 18 and older, found the booster shots to be at least 56% effective against Covid-related visits to emergency departments or urgent care centers and hospitalizations, compared with unvaccinated people.”
There’s some interesting data comparing mortality rates among unvaccinated patients between the Delta and Omicron strains. Overall, there appears to be a lower risk of death among hospitalized unvaccinated patients during the Omicron strain compared to the Delta strain. Among both Omicron and Delta infections, patients with a history of vaccination or prior COVID infection had half the risk of severe disease or death compared to those unvaccinated or without prior infection, and this rate did not change between the two strains.
I’m not going to lie, it’s been kind of a tough week for emergency medicine. I won’t even get into the Medicare reimbursement cuts or the story that NYU ER gives preferential treatment to VIPs. The biggest issue was the diagnostic error data published by the AHRQ that CNN and the NY Times did stories on. The headline you may have come across is that 250,000 people die in the ER each year due to misdiagnosis. We are human and not perfect, but the study was flawed–looking at 20 years worth of papers, including using data from outside the US where physicians were not emergency medicine trained. Prior to the publication of the study, experts pointed out the methodology flaws and expressed concerns about eroding public trust. And even with the methodology issues, serious harm was noted in only 0.3% of patients and deaths in 0.2% of patients. (If you want to read more of the details, I’ve posted some tweets, @drmikesilverman, on the subject). There was also a $10.1 million jury verdict in Texas for delays in care that led to a women’s paralysis. It’s an unfortunate case with a bad outcome and admittedly, I don’t know all the details. However, from what’s been published, the timeline appears extraordinarily efficient for the real world and sets a challenging bar for those of us practicing medicine to achieve. We all realize mistakes and delays occur, but this kind of case gives the practicing physician pause thinking that we can held responsible for bad outcomes even when things are done well. Ending the week was a story about how Maryland ER wait times are the worst in the country. This isn’t VHC but hits close to home, and I know how hard my friends and colleagues are working around the state to provide care to patients.
I’m looking forward to some time with family and friends over the weekend and I hope everyone has a wonderful holiday and gets some time to celebrate over the next week. Stay warm. I’m taking next Friday off from posting so have a happy New Year’s too and I’ll see in in 2023.
Coronavirus is not quite done with us yet.
Science matters. Get vaccinated (or your booster). Keep a mask handy.
Mike