Thanks as always to Dr. Mike Silverman, Chair of the Department of Emergency Medicine at the Virginia Hospital Center in Arlington, for these superb updates!
Friday Night Update from the ER in Arlington, VA
ER volumes remain really high. We closed out last week with another record week when it comes to volume. That was back to back weeks of the highest volumes we’ve seen in a 7 day period. These are not records we want to set. With that said, we’re doing a ton of COVID testing since so many patients are presenting with fever, cough, shortness of breath, and other flu-like (or COVID-like) symptoms. Fortunately, our COVID numbers have not increased and our percent positive rate has also been steady. We are seeing a lot of flu.
We’ve seen an increase in the number of patients requiring our isolation protocols over the last few weeks. This correlates with the increased number of patients we’ve caring for in the ER the last 3 weeks as well, and certainly patients presenting with flu and RSV will also require isolation status until testing is complete. Fortunately, while the number of people requiring hospitalization has also increased, it’s not proportional to the volume. A higher percentage of patients who were in isolation status are able to go home the last few weeks than in weeks previous. Admission rates declined from 38% to 32% over the last month.
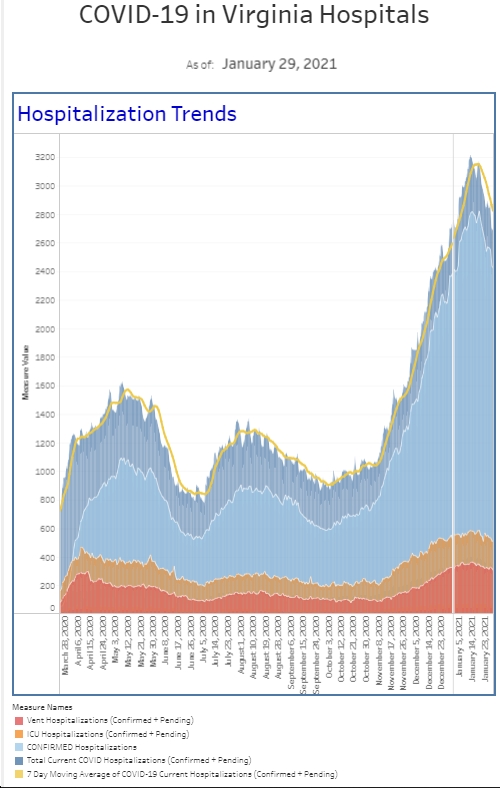
Our COVID inpatient volume is also down about 10% compared to last week. Though the number is still in what I consider our normal range, but down is better than up.
I haven’t hit on much COVID literature recently so let me cover a few topics since COVID is still with us and unlikely to disappear in the near future. And since most people I know have had COVID at least once and many people I know have had COVID a two or more times, the first article is particularly timely. Published this week in Nature, authors used a VA patient population of over 400,000 patients who had COVID at least once and over 40,000 patients with two or more COVID infections and compared them to over 5 million patients who had not had COVID. The authors found “that patients with reinfections tended to have more complications in various organ systems both during their initial illness and longer term, and they were more likely to be diagnosed with long covid than people who did not get another infection.” These findings also “applied regardless of people’s vaccination status or whether they were boosted.” Yes, VA patients tend to be older and perhaps sicker than a non-VA adult patient population but the authors performed risk stratification to account for this.
In the NEJM this week, authors looked at the impact of lifting universal masking in school and on COVID infections rates. I’m tired of wearing masks in meetings and I know my son was so happy to take his mask off at school, but in this study, the conclusions were clear: “Among school districts in the greater Boston area, the lifting of masking requirements was associated with an additional 44.9 Covid-19 cases per 1000 students and staff during the 15 weeks after the statewide masking policy was rescinded.”
Published about 2 weeks ago in Clinical Infectious Diseases, authors looked at a population of 12 million people in Ontario, Canada and found that social determinants of health “including lower socioeconomic status and a higher proportion of racially minoritized groups, correlated with higher likelihood of COVID-19-related death.” We clearly saw this early in the pandemic and while it’s not making the news anymore, it doesn’t mean that social determinants of health won’t continue to have an impact on morbidity and mortality.
And finally, in our COVID news update, there is a new treatment available for hospitalized COVID pneumonia patients who require oxygen and are at risk of progressing to severe respiratory failure. The FDA has issued Emergency Use Authorization for Anakinra Injection, which is “an interleukin-1 (IL-1) receptor antagonist that is currently FDA approved for treatment of rheumatoid arthritis, cryopyrin-associated periodic syndromes, and deficiency of IL-1 receptor antagonist.” It’s great that we continue to have to ways to fight COVID pneumonia because even though hospital numbers are lower than last winter, people are still dying of COVID.
Yesterday, I was honored to receive the Spirit of Community Award from the Arlington Community Foundation. I was one of three winners and the other two were really inspirational. It was a great event, and I was thrilled to have such a large turnout from my VHC family (see photo). I am incredibly happy that so many people have read and appreciated these posts over the last 2 ½ years. I certainly never expected to be recognized in any way for writing these posts.
Coronavirus is not quite done with us yet.
Science matters. Get vaccinated (or your booster). Keep a mask handy.
Mike